|
India healthcare system has made commendable progress in recent decades, but challenges such as accessibility, affordability, infrastructure gaps, and disease burden persist. With a population exceeding 1.4 billion, transforming healthcare into a robust, inclusive, and efficient system is not just a public welfare imperative—it is a strategic necessity for national development.
As the country navigates the post-pandemic landscape, the focus has shifted towards creating a resilient, technology-driven, and equitable healthcare system that serves both urban elites and rural poor alike.
Current Status of India Healthcare System
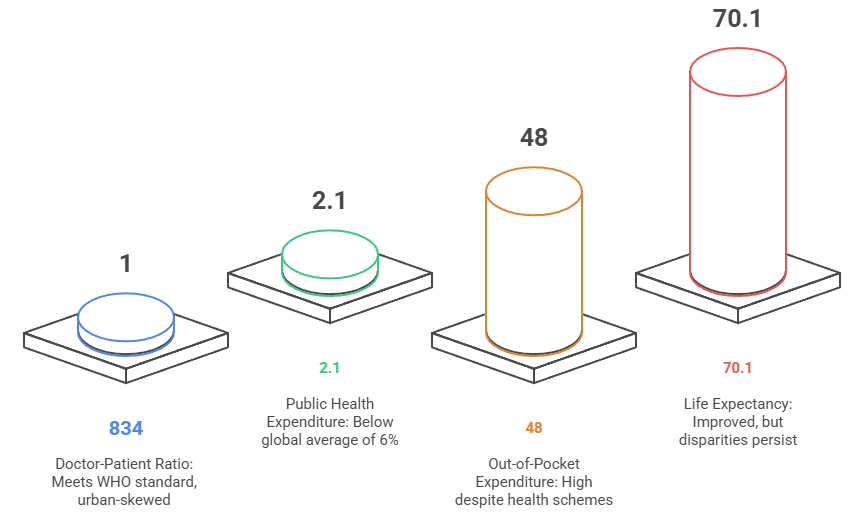
- Doctor-Patient Ratio: India has 1 doctor for every 834 people (as per the National Health Profile 2023), which meets the WHO standard of 1:1000, but the distribution remains skewed towards urban areas.
- Public Health Expenditure: Government spending on health is around 2.1% of GDP (2023–24), still below the global average of 6%.
- Out-of-Pocket Expenditure (OOPE): Despite schemes like Ayushman Bharat, over 48% of total health spending in India is still borne out-of-pocket by households.
- Life Expectancy: Improved to 70.1 years (World Bank, 2023), but disparities remain across states and social groups.
Major Challenges in India Healthcare Landscape
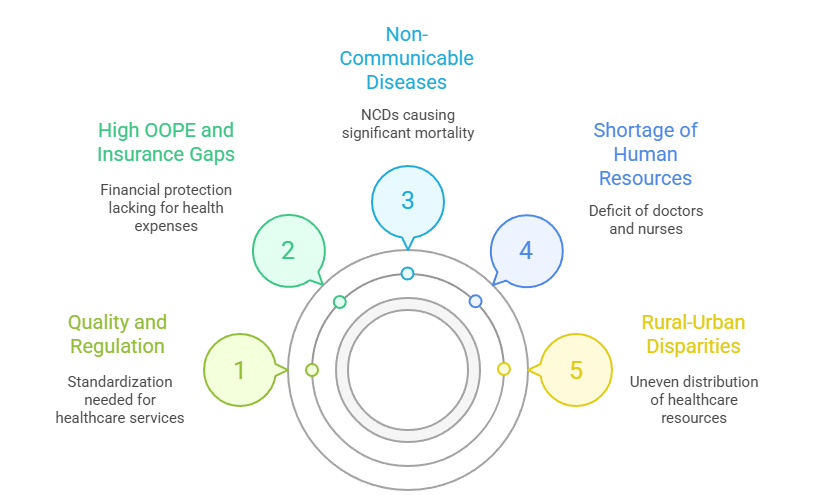
- Rural-Urban Disparities
- Over 65% of India population lives in rural areas, but most doctors, specialists, and hospitals are concentrated in cities.
- Primary Health Centres (PHCs) and Community Health Centres (CHCs) often face a shortage of staff, medicines, and equipment.
- Shortage of Human Resources
- India faces a deficit of over 6 lakh doctors and 2 million nurses (as per NITI Aayog estimates).
- The doctor-to-patient and nurse-to-patient ratios are worse in tribal and backward regions.
- Non-Communicable Diseases (NCDs)
- NCDs like diabetes, hypertension, and cancer account for over 65% of all deaths in India.
- Lack of regular screening and poor awareness leads to late-stage diagnosis, increasing treatment costs.
- High OOPE and Insurance Gaps
- A significant percentage of the population lacks financial protection, making catastrophic health expenses a common cause of poverty.
- Only about 37% of Indians have any form of health insurance.
- Quality and Regulation
- The unregulated private sector caters to over 70% of outpatient care and nearly 60% of hospital care, but often lacks standardization in pricing and quality.
Government Initiatives Transforming Healthcare
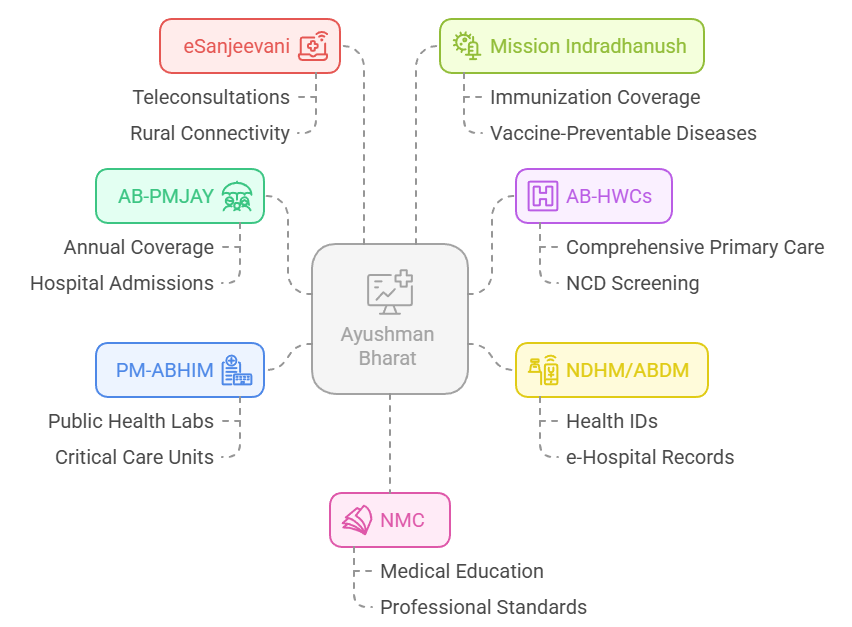
Ayushman Bharat – Pradhan Mantri Jan Arogya Yojana (AB-PMJAY)
- Launched in 2018, it is the world’s largest health insurance scheme, offering Rs. 5 lakh annual coverage per family to over 12 crore poor and vulnerable families.
- As of 2024, over 6 crore hospital admissions have been facilitated under the scheme.
Ayushman Bharat – Health and Wellness Centres (AB-HWCs)
- Over 1.7 lakh HWCs have been operationalized as of mid-2024, offering comprehensive primary care, including NCD screening, maternal and child health, and mental healthcare.
National Digital Health Mission (NDHM) / Ayushman Bharat Digital Mission (ABDM)
- Aims to create a digital health ecosystem with components like Health IDs, e-Hospital records, e-Pharmacy, and teleconsultation.
- Over 50 crore Health IDs have already been issued.
PM Ayushman Bharat Health Infrastructure Mission (PM-ABHIM)
- Announced in 2021 with an outlay of Rs. 64,180 crore, it seeks to strengthen public health labs, critical care units, and emergency response systems across the country.
eSanjeevani Telemedicine Platform
- India’s flagship teleconsultation platform, with over 16 crore consultations completed by 2024.
- Especially effective in connecting rural populations with urban specialists.
Mission Indradhanush & Intensified MI
- Immunisation drive targeting children and pregnant women; coverage has crossed 90% in many districts, significantly reducing vaccine-preventable diseases.
National Medical Commission (NMC)
- Replaces the MCI to ensure transparency in medical education and professional standards, encouraging expansion of medical colleges and quality training.
Emerging Trends and Innovations

Public-Private Partnerships (PPPs)
- Several state governments (like Gujarat, Rajasthan, and Andhra Pradesh) are leveraging PPPs to improve access and quality of care, especially for diagnostics and dialysis.
Telemedicine and AI Integration
- AI-based diagnostic tools and remote health monitoring are being piloted in many government programs to enhance early detection and resource optimization.
Promotion of AYUSH Systems
- India is promoting traditional systems of medicine—Ayurveda, Yoga, Unani, Siddha, and Homeopathy—with the creation of AYUSH health centres and research institutes under the Ministry of AYUSH.
Case Study: Mohalla Clinics and Delhi Model
The Mohalla Clinics in Delhi serve as an example of accessible, low-cost, primary healthcare delivery at the community level. These clinics offer free consultations, medicines, and diagnostics, and have been replicated in other states like Telangana and Punjab.
Recommendations for a Future-Ready Healthcare System
- Increase Public Health Spending
- Raise expenditure to at least 2.5% of GDP by 2025 (as per National Health Policy 2017 target).
- Expand Insurance Coverage
- Integrate informal workers and middle-class families under universal health coverage.
- Strengthen Primary Healthcare
- Invest in human resources, supply chains, and digital infrastructure at the grassroots level.
- Regulate and Standardize the Private Sector
- Implement pricing caps, quality audits, and grievance redressal systems for private hospitals and labs.
- Focus on Preventive and Mental Healthcare
- Promote lifestyle changes, awareness campaigns, and destigmatize mental health services.
- Bridge the Rural-Urban Divide
- Incentivize medical professionals to work in rural and remote areas, and improve infrastructure and connectivity.
Conclusion
India’s healthcare transformation is at a critical juncture. While visionary schemes like Ayushman Bharat, digital health missions, and infrastructure investments have laid a strong foundation, sustained efforts are essential to ensure healthcare for all—not just in policy, but in practice.
A holistic, inclusive, and technology-enabled approach can turn India’s healthcare system into a model of resilience and equity, capable of not only treating disease but also fostering well-being, productivity, and social justice across the nation.
|







One comment