Introduction
Public health interventions in India hold profound sociological importance, as they not only prevent disease but also address questions of equity, access, and social justice. The Universal Immunisation Programme (UIP)—the world’s largest vaccination drive—reflects India’s commitment to safeguarding maternal and child health. Each year, it vaccinates around 2.6 crore infants and 2.9 crore pregnant women, offering protection against multiple life-threatening diseases.
Despite achievements such as polio eradication and tetanus elimination, rural–urban divides, vaccine hesitancy, and systemic barriers continue to produce health inequalities. Analysing UIP through a sociological lens highlights how class, caste, gender, and regional disparities intersect with public health outcomes.
Historical Evolution
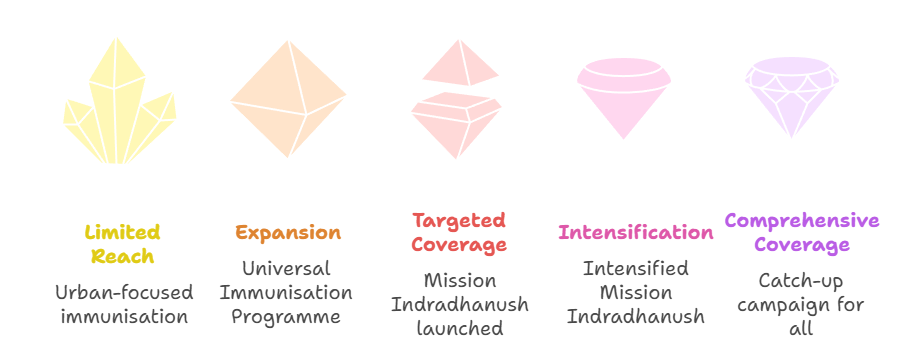
- 1978: Launched as the Expanded Programme on Immunisation, focused mainly on urban areas.
- 1985: Rebranded as the Universal Immunisation Programme, expanding to rural India.
- 2014: Mission Indradhanush launched to cover unvaccinated children.
- 2017 onwards: Intensified Mission Indradhanush (IMI) expanded to reach missed populations.
- 2023: IMI 5.0 conducted as a catch-up campaign for children up to 5 years and pregnant women.
Sociological view: This historical trajectory mirrors India’s broader development story—moving from elitist, urban-centric interventions to inclusive, rights-based public health expansion.
Status of Immunisation in India
The UIP today offers free immunisation against 12 diseases:
- Nationally: Diphtheria, Pertussis, Tetanus, Polio, Measles, Rubella, Tuberculosis, Hepatitis B, and Haemophilus Influenzae type B.
- Region-specific: Rotavirus, Pneumococcal Pneumonia, and Japanese Encephalitis.
Coverage: India reports 98% full immunisation coverage (FY 2024-25)—a remarkable leap, though gaps remain in disadvantaged clusters.
Technological tools:
- eVIN (Electronic Vaccine Intelligence Network): Real-time monitoring of vaccine stocks.
- U-WIN platform: End-to-end digital registration and tracking, ensuring migrant populations are not left behind.
Key Achievements
- Polio eradication (2014): A milestone in global health.
- Yaws-free status (2016) and Maternal & Neonatal Tetanus elimination (2015): Achieved ahead of global targets.
- Digital innovations: Building on Co-WIN, U-WIN now provides universal tracking.
Sociological significance: These successes illustrate state capacity (Michael Mann), collective action (Durkheim), and the ability of science and technology to generate “social solidarity” in fighting epidemics.
Challenges to Universal Immunisation

- Geographic Exclusion
- Remote, tribal, and conflict-ridden areas remain underserved.
- Weak infrastructure hinders access in UP, Bihar, and parts of the Northeast.
- Reflects spatial inequality—a form of structural marginalisation.
- Vaccine Hesitancy
- Stems from misinformation, cultural beliefs, and distrust in state institutions.
- Can be linked to Weber’s concept of traditional authority, where local healers may command more trust than medical science.
- Pandemic Disruptions
- COVID-19 diverted resources and interrupted routine immunisation, causing resurgent measles outbreaks.
- Illustrates how global crises exacerbate local vulnerabilities.
- Low Awareness & Social Stratification
- Marginalised groups (slum dwellers, migrants, Dalits, minorities) often miss out.
- Pierre Bourdieu’s concept of cultural capital helps explain why illiteracy and low awareness create barriers to accessing healthcare.
- Gender Inequality
- Mothers in patriarchal households may lack autonomy to take children for vaccination.
- Ties to Sylvia Walby’s patriarchy theory, where women’s reproductive roles are socially undervalued.
Sociological Perspectives
- Functionalism (Durkheim)
- UIP strengthens collective solidarity by protecting vulnerable populations, enhancing social integration, and preventing epidemics.
- Conflict Perspective (Marx)
- Unequal access to vaccines mirrors class and caste hierarchies.
- Privatization of healthcare may deepen inequalities between elites and rural poor.
- Structural-Functional Approach (Parsons)
- Health is key to maintaining the “social system.” Immunisation ensures individuals fulfil social roles by preventing illness.
- Post-colonial and Indian Perspectives
- B.R. Ambedkar: Unequal access to health services perpetuates caste oppression.
- Amartya Sen: Health is a capability; immunisation enhances freedom to live a healthy life.
Measures to Bridge Gaps
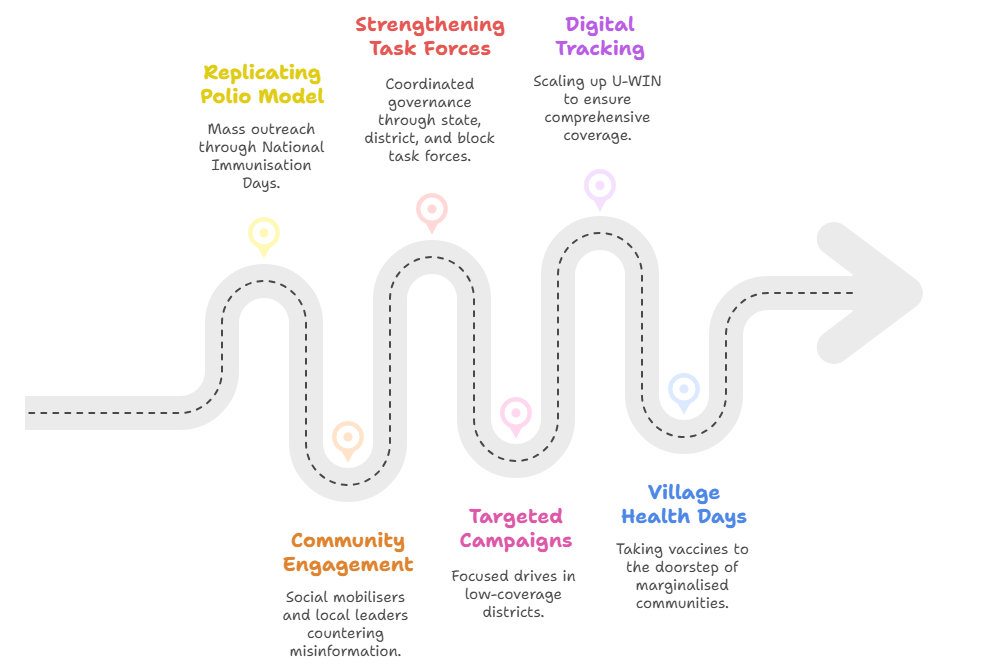
- Replicating Pulse Polio Model
- Mass outreach through National Immunisation Days.
- Community Engagement
- Social mobilisers, local leaders, and SHGs to counter misinformation.
- Strengthening Task Forces
- State, District, and Block Immunisation Task Forces for coordinated governance.
- Targeted Supplementary Campaigns
- Focused drives in low-coverage districts.
- Digital Tracking
- Scaling up U-WIN to ensure every child and pregnant woman is covered.
- Village Health & Nutrition Days
- Taking vaccines to the doorstep of marginalised communities.
Conclusion
India’s Universal Immunisation Programme demonstrates how public health can be both a biomedical and sociological project. While remarkable achievements highlight the success of state-led interventions, persistent challenges—vaccine hesitancy, social inequality, geographic exclusion—underscore the need for deeper engagement with communities.
For India to achieve true universality, immunisation must be seen not just as a health programme but as a social justice imperative, addressing the structural inequalities that leave certain groups behind.
|





3 comments